A little girl, not more than three years old, touches the lifeless body of her seven-year-old sister who has just succumbed to Ebola. She cries when her sister does not respond. They are both in the isolation ward at the Kailahun Treatment Centre at the epicenter of the Ebola crisis in eastern Sierra Leone. With the death of the last member of her family, the little girl’s world has shrunk. Who knows, if it will close in on her as well.
It’s a heart-breaking scene, but Esther Wanjiru, a volunteer doctor from Kenya with Medecins Sans Frontières, or Doctors Without Borders, has witnessed it many times over the last few months.
“Just days earlier, we had to prise the seven-year-old away from her little sister. They didn’t want to be separated, but both were very ill and [the older] simply became too sick to continue caring for the little one,” says Wanjiru.
Each time death comes calling at this Ebola camp, Wanjiru says it’s a terrible experience.
“When you watch this on television, these are Ebola patients. But when you are here, these are families suffering great tragedy.”
Wanjiru, 27, is on the frontline of the Ebola crisis along with countless other volunteer doctors who are putting their lives at risk to care for the sick and dying.
It’s a mammoth task trying to contain a virus that has the potential to decimate whole populations in days.
Wanjiru arrived in Kailahun District in July for a second mission with Doctors Without Borders. On her first mission, she had been shaken by the sight of the isolation wards.
“I had never seen anything like it before,” she says. However, returning yet again to the wards, she hopes the African public understands the magnitude of the Ebola scare.
“It’s high time the world woke up, this virus has spread so fast.”
The virus, Wanjiru claims, takes away more than a victim’s life and its ramifications are not stated enough.
“I quickly realized there are many factors, it’s not just about isolation wards, but about kids being left alone, communities who are afraid and patients being left to die in their homes. These are things that are not being addressed. Pledges are not enough, we need people in the field, we need more people hands-on.”
Wanjiru fears for her life, every day.
“Yes of course I’m scared, it’s one of the deadliest diseases on earth. When I left for the mission, my family thought I was crazy. But as a doctor, I thought if I can help in any way, why not? This virus can affect many countries and by doing this, I’m also helping protect my family, my friends and my country,” she says.
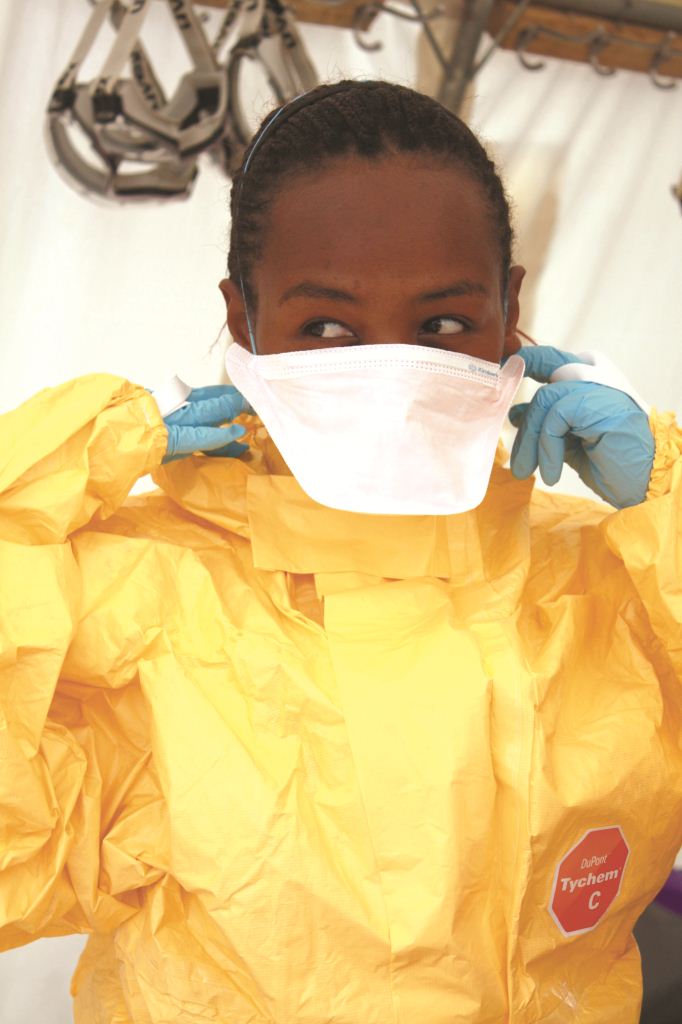
After her arrival, Wanjiru was briefed on the dangers and procedures in the field. And although she does not don the most convenient – or flattering – of ensembles, she is now used to the protective gear.
“Luckily it’s not that hot at the moment. I find the most difficult part of the clothing is having my face covered, but if it gets too much, I go outside for a break.”
The doctor works an 80-hour week, sometimes more when on call. Wanjiru’s day consists of ward rounds and daily briefings. And despite the long hours, she says she wakes up thinking about her patients from the previous day. Death is a constant here.
She remembers a toddler and his mother, both of who survived and were reunited. Their survival is a small triumph.
Wanjiru returns to Kenya in October and is looking forward to having chapatis (Indian bread) again. But the trip home may be temporary. The young doctor says she’s willing to return to the ward “in a heartbeat”.